DISCOVERIES REPORTS (ISSN 2393249X), 2022, volume 5
REVIEW ARTICLE
CITATION: Mungalpara N., Patel N., Mehta A. A case report of ultrasound-guided peri-ligamentous steroid injection for grade 1 ankle sprain in elite kabaddi athlete. Discoveries Reports 2022; 5(3): e35. DOI: 10.15190/drep.2022.9
Submitted: Aug 04, 2022; Revised: Sep 13, 2022; Accepted: Sep 13, 2022; Published: Dec 31, 2022;
A case report of ultrasound-guided peri-ligamentous steroid injection for grade 1 ankle sprain in elite kabaddi athlete
Nirav Mungalpara 1, *, Nishil Patel 2, Aditya Mehta 3
1 Medicircle Private Limited, Vidyavihar West, Mumbai, India
2 BJ Medical College, Asarwa, Ahmedabad, Gujarat, India
3 Shantaba Medical College, Amreli, Gujarat, India
* Corresponding authors:
Dr. Nirav Mungalpara, Medicircle Private Limited, Vidyavihar West, Mumbai 400086, India; Email: nirav.orthodoc@gmail.com
Abstract
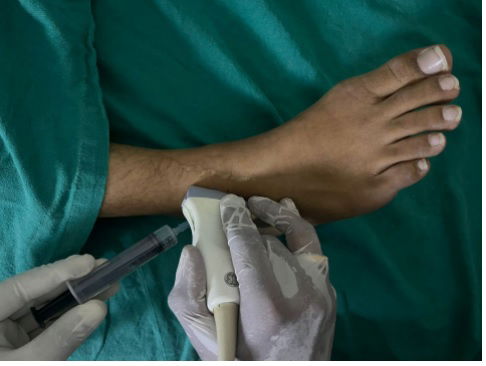
The role of using local steroid administration for acute grade 1 ankle ligament injury is debatable. Here, we are presenting a case of an elite kabaddi athlete who sustained this type of injury in an international kabaddi tournament. To facilitate the functional recovery and return to play, a peri-ligamentous local steroid under ultrasound guidance was given. Numerical Pain Rating Score (NPRS) has improved nearly 70% after the first 48 hours from the intervention, helping him to progress very rapidly in his rehabilitation program. Although World Anti-Doping Agency (WADA) has recently placed local steroid injections under strict scrutiny, they are still a viable option when carefully selected. A higher level of evidence is required to confirm this intervention.
Access FULL text of the manuscript here: FULL ARTICLE (PDF)
REFERENCES
1. Yallappa M, A study on common injuries of Kabaddi players, International Journal of Physical Education, Sports and Health 2020; 7(3): 37-43
2. World Anti-Doping Agency, The World Anti-doping Code. The 2022 Prohibited List, International Standard, 2022 Retrieved from: https://www.wada-ama.org/sites/default/files/ resources/files/2022list_final_en.pdf
3. Chang CW, Huang TY, Tseng YC, Chang-Chien GP, Lin SF, Hsu MC. Positive doping results caused by the single-dose local injection of triamcinolone acetonide. Forensic Sci Int. 2014;244:1-6. doi:10.1016/j.forsciint.2014.07.024
4. Bleakley CM, Glasgow P, MacAuley DC. PRICE needs updating, should we call the POLICE?. Br J Sports Med. 2012;46(4):220-221. doi:10.1136/bjsports-2011-090297
5. Chuang LL, Wu CY, Lin KC, Hsieh CJ. Relative and absolute reliability of a vertical numerical pain rating scale supplemented with a faces pain scale after stroke [published correction appears in Phys Ther. 2016 Jun;96(6):917]. Phys Ther. 2014;94(1):129-138. doi:10.2522/ptj.20120422
6. Lynch SA, Renström PA. Treatment of acute lateral ankle ligament rupture in the athlete. Conservative versus surgical treatment. Sports Med. 1999;27(1):61-71. doi:10.2165/00007256-199927010-00005
7. Hertel J. Functional Anatomy, Pathomechanics, and Pathophysiology of Lateral Ankle Instability. J Athl Train. 2002;37(4):364-375.
8. Milner CE, Soames RW. Anatomy of the collateral ligaments of the human ankle joint. Foot Ankle Int. 1998;19(11):757-760. doi:10.1177/107110079801901109
9. Golanó P, Vega J, de Leeuw PA, et al. Anatomy of the ankle ligaments: a pictorial essay. Knee Surg Sports Traumatol Arthrosc. 2010;18(5):557-569. doi:10.1007/s00167-010-1100-x
10. Hughston JC. The importance of the posterior oblique ligament in repairs of acute tears of the medial ligaments in knees with and without an associated rupture of the anterior cruciate ligament. Results of long-term follow-up. J Bone Joint Surg Am. 1994;76(9):1328-1344. doi:10.2106/00004623-199409000-00008
11. Chapman MW. Chapman's Orthopedic Surgery. Lippincott Williams and Wilkins (LWW) 2000:2473–83.
12. Aradi AJ, Wong J, Walsh M. The dimple sign of a ruptured lateral ligament of the ankle: brief report. J Bone Joint Surg Br. 1988;70(2):327-328. doi:10.1302/0301-620X.70B2.3126191
13. Kaminski TW, Hertel J, Amendola N, et al. National Athletic Trainers' Association position statement: conservative management and prevention of ankle sprains in athletes. J Athl Train. 2013;48(4):528-545. doi:10.4085/1062-6050-48.4.02
14. Wolfe MW, Uhl TL, Mattacola CG, McCluskey LC. Management of ankle sprains [published correction appears in Am Fam Physician 2001 Aug 1;64(3):386]. Am Fam Physician. 2001;63(1):93-104.
15. Stephens MB, Beutler AI, O'Connor FG. Musculoskeletal injections: a review of the evidence. Am Fam Physician. 2008;78(8):971-976.
16. Nichols AW. Complications associated with the use of corticosteroids in the treatment of athletic injuries. Clin J Sport Med. 2005;15(5):370-375. doi:10.1097/01.jsm.0000179233.17885.18
17. Lai MWW, Sit RWS. Healing of Complete Tear of the Anterior Talofibular Ligament and Early Ankle Stabilization after Autologous Platelet Rich Plasma: a Case Report and Literature Review. Arch Bone Jt Surg. 2018;6(2):146-149.
18. Blanco-Rivera J, Elizondo-Rodríguez J., Simental-Mendía M, Vilchez-Cavazos F., Peña-Martínez V. M, Acosta-Olivo C. Treatment of lateral ankle sprain with platelet-rich plasma: A randomized clinical study. Foot and ankle surgery: of icial journal of the European Society of Foot and Ankle Surgeons. 2022; 26(7), 750–754. https://doi.org/10.1016/j.fas.2019.09.004